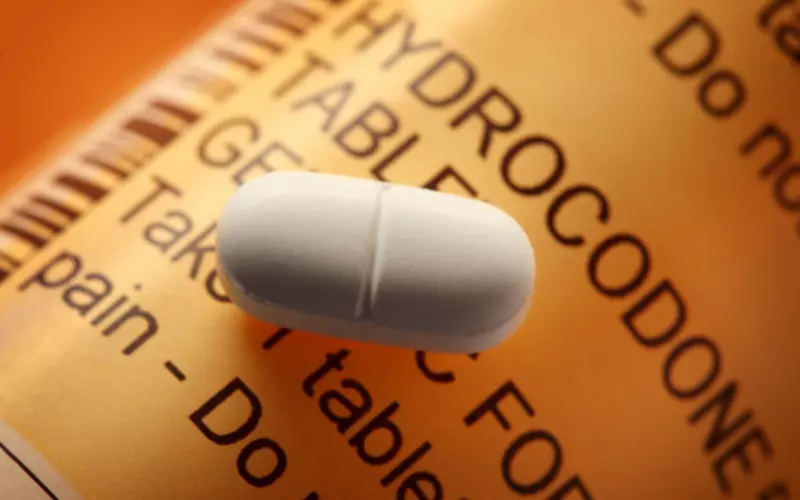
How Long Does Vicodin Stay in Your System?
Vicodin is a popular opioid painkiller that treats moderate to severe pain. Usually, people receive a prescription after oral surgery or outpatient procedures to treat

Vicodin is a popular opioid painkiller that treats moderate to severe pain. Usually, people receive a prescription after oral surgery or outpatient procedures to treat

The dangers of mixing alcohol and vicodin can be life-threatening. Learn more about the side effects and how to spot the signs of opioid painkillers abuse.
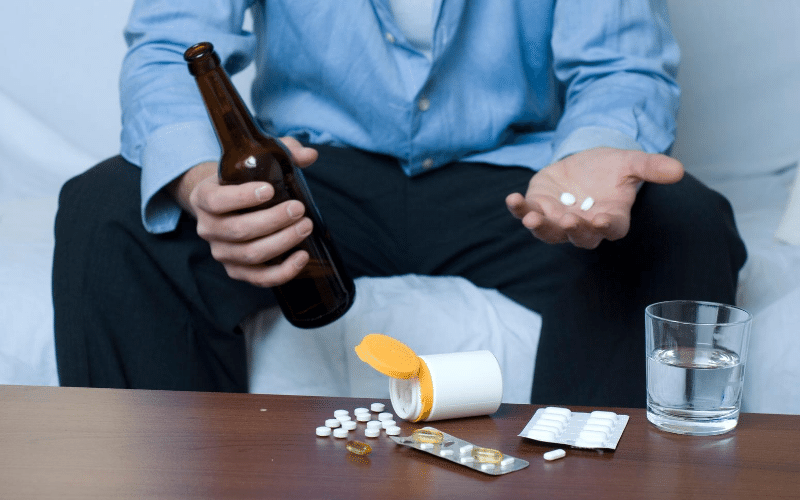
Mixing Alcohol and Prescription Painkillers It has become pretty common knowledge that mixing alcohol and prescription pills is a lethal practice, what with all of
In this day and age, it is extremely commonplace for doctors to jot down and hand out prescription medication – often without any questions or

Vicodin and Alcohol Simply put, mixing Vicodin and alcohol is a recipe for disaster. The two chemicals interact with each other in such a way

With the FDA approving, Hysingla ER, a new abuse-proof painkiller, can painkillers addictions be coming to an end? Learn everything you need to know.
Painkiller Addiction Facts and Statistics Painkiller addiction is nothing new. Ancient cultures all over the world used opium, both to treat pain and to catch
866-308-2090
1609 S Congress Ave
Boynton Beach, FL 33426
Lighthouse Recovery Institute treatment center is close to the beaches in gorgeous Boynton Beach, FL, Learn more